Retained Foreign Body Cellulits SplinterRetained foreign bodies and puncture wounds of the hand are very common.
Assessment of a patient with a puncture wound and suspected foreign body begins with a careful history and physical examination. Patients who present with a wound or localized pain following penetrating trauma should be questioned regarding the specific timing and nature of the injury, the level of wound contamination and any materials involved in the injury. Foreign bodies are most commonly composed of wood, glass, or metal. A careful assessment of the patient’s current symptoms should be sought, including the location, quality, severity and radiation of pain, the presence of a foreign body sensation, signs of infection including; swelling, warmth, or redness to the wound and any neurologic symptoms (including motor or sensory deficits).
If exploration and surgical removal of a foreign body of a puncture wound is necessary, it should be performed under sterile conditions, adequate anesthesia and tourniquet control. Infection is very commonly associated with puncture woulds and retained foreign bodies. Appropriate antibiotic treatment is recommended.
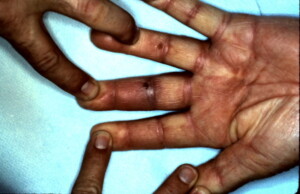 Puncture wound at the proximal inter-phalangeal joint flexion crease with a piece of wood was sustained in this patient.
Puncture wound at the proximal inter-phalangeal joint flexion crease with a piece of wood was sustained in this patient.
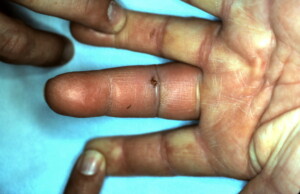 Erythema, tenderness and warmth of the digit was evident and fear of a flexor tenosynovitis was present therefore patient was taken to the operating room for exploration, removal of foreign body and copious irrigation. Violation of the flexor sheath was not sustained so purulent flexor tenosynovitis was not present.
Erythema, tenderness and warmth of the digit was evident and fear of a flexor tenosynovitis was present therefore patient was taken to the operating room for exploration, removal of foreign body and copious irrigation. Violation of the flexor sheath was not sustained so purulent flexor tenosynovitis was not present.
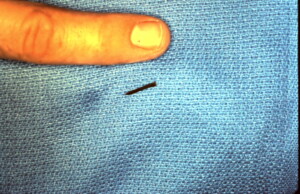 Foreign body was identified and removed. It is shown next to my finger for size comparison. IV antibiotics were administered pre-operatively and oral antibiotics continued post-operatively.
Foreign body was identified and removed. It is shown next to my finger for size comparison. IV antibiotics were administered pre-operatively and oral antibiotics continued post-operatively.



